by Lilian van der Ven, MD, Amsterdam UMC

In the Netherlands, a physician who has passed the final examinations in medicine can pursue training in an area of medical specialization. There are four types of specialist training: General Practitioner: 3 years; Specialist: 4-6 years; Public Health Specialist: 2.5-4 years and Nursing Home Specialist: 2 years.
Public Health Specialist: Most physicians who apply to train in public health are already employed in one of the branches of public health medicine. If not, the trainee must find a job that meets the approval of the SRC, so the trainee can receive appropriate support during practice training. The employer pays for most of the cost of training. In The Netherlands, the term ‘social medicine’ is used to describe the part of medicine that focuses on the interaction between health and the environment, both individually and at group/community level.
As for the relationship between social medicine and public health: the social medicine specialist can be seen as the doctor in the field of public health, and the public health worker in the field of medicine.
Social medicine is a broad field with two main branches: employment & health (E&H) and society & health (S&H). Employment & health (E&H) is further divided into two branches – occupational health and insurance health.
S&H is further divided into eight profiles: Youth public health, Infectious disease control, Forensic medicine, Tuberculosis control, Environmental health, Social medical assessment and advice, Policy and advice and Donor medicine.
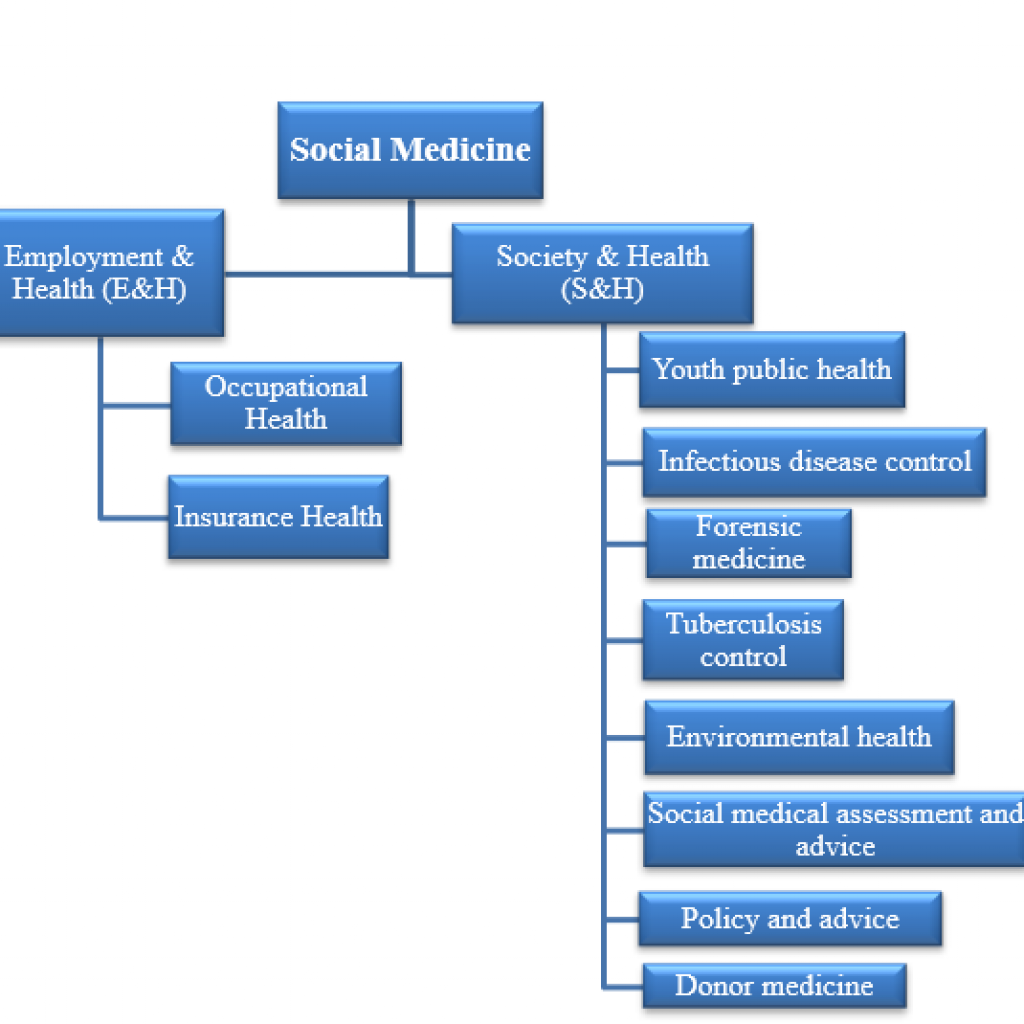
Prospective specialists can choose which branch or profile they want to be trained in. It is not uncommon for a specialist to be trained in multiple profiles, for example infectious disease control and forensic medicine.
Social medicine training in the Netherlands
Pre-training requirements
The residency program is open to those who have completed six years of medical school. After these six years, graduates usually start working in a field they are interested in, for example employed by a municipal health service or an occupational health & safety service.
The employer then decides if their employee can apply for a spot in the residency program. Sometimes the start of employment and the start of residency will coincide, in other cases the prospective resident will gain some working experience before being allowed to start the residency.
Duration of training
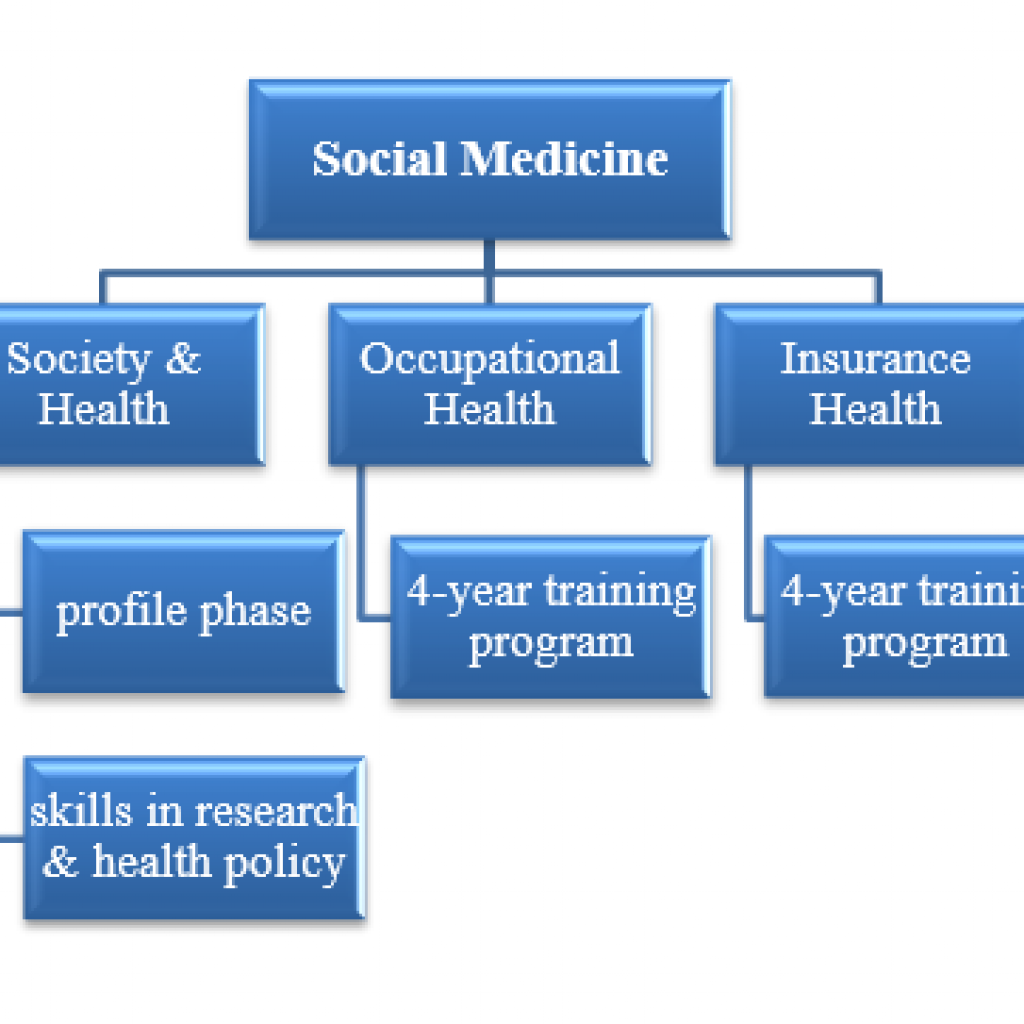
As described above, the field of social medicine is divided into three branches: society & health, occupational health and insurance health. Each branch has its own residency program. There are three schools that offer these programs.
The residency for society & health is divided into 2 two-year phases.
Phase 1 is the profile phase, where residents acquire skills that are relevant to their chosen profile.
Phase 2 is a more overarching phase that focuses on skills in research and health policy. It is not mandatory for residents to complete both phases.
However, to become a social medicine specialist one does have to complete the full four years; residents that have only completed the first phase are called profile doctors.
For both occupational health and insurance health there is a four-year training program.
Mandatory educational requirements
Currently, most residents remain employed by the same employer they started working with for the entire duration of the residency. There are no rotations. The resident is expected to gain his professional skills in this workplace. There is some room for elective internships, but this is limited, for example a total of twelve weeks for residents in insurance health.
Theoretical education takes place in modules that differ between profiles and branches. Some modules focus specifically on skills that are relevant to a particular profile or branch. However, all residency programs also include modules that focus on overarching topics like research, epidemiology, health policy making, health systems, innovation and management. There is some room for elective modules. During residency, the resident is supervised by two mentors; one from the public health school and one from the workplace.
End of training assessment
The training program is based on the CanMEDS competencies. In order to become a social medicine specialist, residents must prove they have gained all competencies specified. They have to prove this by building a portfolio, consisting of written assignments, presentations, assessments on different aspects of their practical work, reports on elective interships and training, self-assessments and self-evaluations, and assessments and evaluations by the mentors. The end of the residency consists of an interview with both mentors, during which the mentors evaluate if the resident has gained all competencies and is therefore eligible to become a social medicine specialist.
Interesting websites
- EuroNet MRPH: the website of EuroNet MRPH, the European association of medical residents in public health. More information about the Winter Meeting will be published here
- EuroNet MRPH Winter Meeting 2019: the official website of the EuroNet MRPH meeting
- ARTS MG: information about the residency program in society & health under the new national employership (in Dutch)
- Losgio: website of the Dutch association of residents in social medicine

Citation:
Van der Ven, Lilian: Public Health in The Netherlands: Meeting the Dutch Social Medicine Residents (In: Polak, G. [ed.]: GI-Mail 12, ISSN: 2312-0827 Going International, Vienna 2019)
Here you can download this article.
Published in GI-Mail 10/2019 (English edition). Sign up for GI-Mail here.
Tip: More up to date educational events can be found online in the Education Database »medicine & health«.
